When your doctor first mentions “arteriovenous fistula”, you usually don’t feel ready for all the information that follows. The term actually describes a procedure that creates a safe “access point” to the blood, absolutely necessary for long-term hemodialysis. The guide below is designed to help you understand, at your own pace, what a fistula is, why you need one and how you can take care of it day by day.
From Kidney Failure to Dialysis: Why Vascular Access Becomes Important
The kidneys continuously filter the blood, removing toxins and excess water. In advanced chronic kidney disease, this function gradually declines until the body can no longer clean itself. At this point, hemodialysis takes over part of the kidneys’ work: blood is removed from the body, passed through a filter and then returned to circulation.
For this process to be repeated several times a week, a reliable access point is needed, one that can handle large volumes of blood, high pressure and repeated punctures, year after year. Regular veins in the hand cannot withstand this demand. This is where the need for an arteriovenous fistula arises.
What, Exactly, Is an Arteriovenous Fistula
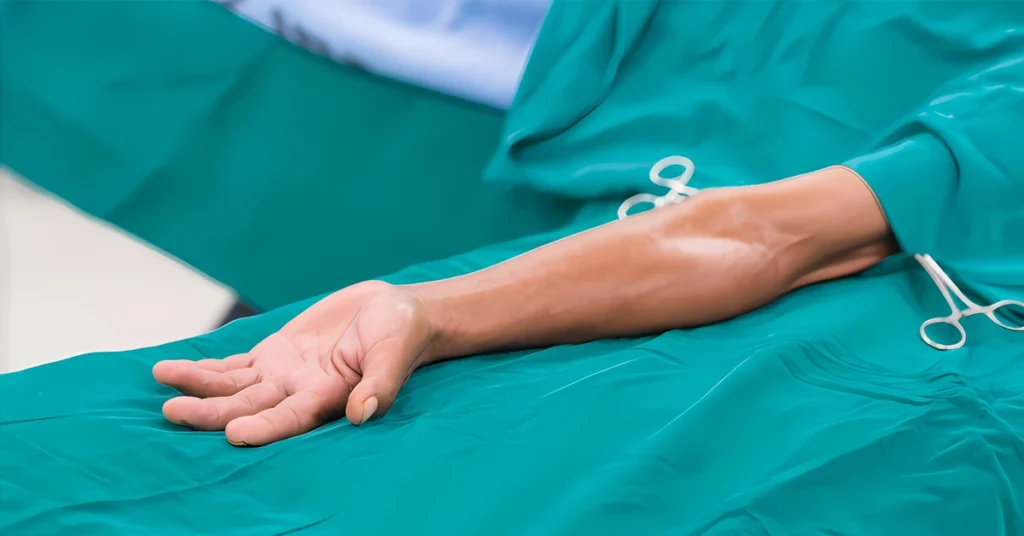
Simply put, an arteriovenous fistula is a surgically created connection between an artery and a vein in the arm. The artery carries blood from the heart at high pressure, while the vein returns it at lower pressure through thinner walls.
When the two are surgically joined, arterial blood begins flowing through the vein at higher pressure. The vein changes over time: its walls thicken, its diameter increases and the vessel becomes more robust. This process, called maturation, usually takes several weeks and transforms the vein into a vessel that can be punctured repeatedly for dialysis sessions.
When the Fistula Conversation Comes Up: Common Scenarios
Doctors do not recommend an arteriovenous fistula to every patient with kidney disease, but specifically to those who are approaching dialysis or are already on a hemodialysis programme. Common situations include:
- Advanced chronic kidney disease, when it is known that dialysis will be needed in the near future;
- Patients on dialysis through a central venous catheter who need a safer long-term solution;
- People for whom early planning of vascular access is desired, several months before the first dialysis session.
The timing and type of fistula are decided by the medical team (nephrologist and vascular surgeon), after assessing both the patient’s general condition and the quality of the blood vessels in the arm.
Types of Fistula: Where It Can Be Placed and What It Means for You
Depending on your vascular anatomy, the doctor may propose several options for fistula placement.
Forearm Fistula
In many cases, the first option is a fistula created near the wrist, between the radial artery and a vein at that level. The advantage is that it keeps the rest of the arm free for future options, and blood flow to the hand is generally well maintained.
Elbow Fistula
If the forearm veins are too thin or damaged, a fistula can be created at the elbow, for example between the brachial artery and the cephalic vein. This type of fistula usually matures faster and provides a higher blood flow, which is useful when dialysis is difficult.
Fistulas for Difficult Anatomy
In patients who have had previous procedures or severely affected veins, other combinations may be used, such as the brachiobasilic fistula with vein transposition. Before any decision is made, a Doppler ultrasound is usually performed to “map” the veins and arteries and identify available options.
What the Fistula Creation Procedure Generally Involves
The procedure is planned in advance and follows several general steps:
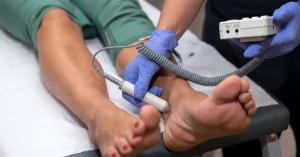
- Pre-operative assessment: blood tests, Doppler ultrasound of the arm vessels and, if needed, additional consultations (for example, cardiology);
- Local or regional anaesthesia: the arm area is numbed so that you feel no pain;
- A small incision: the surgeon accesses the artery and vein through a small cut;
- Connecting the vessels: the artery and vein are joined with a fine suture, performed under optical magnification for precision;
- Checking function: immediately after the suture, the surgeon looks for the “thrill”, the specific vibration that shows blood is flowing through the fistula;
- Dressing and monitoring: after the procedure, the arm is dressed and the patient is monitored for a short period.
The procedure usually lasts no more than a few hours, including preparation and the post-operative observation period.
The First Weeks with a Fistula: What You Will Feel and What to Watch For
In the immediate period after surgery, it is normal to experience mild discomfort or swelling around the incision. As the wound heals, these symptoms reduce.
The most important thing you can do is check the thrill daily: the fine vibration felt when you place your fingers over the fistula area. The constant presence of this vibration is a good sign. A sudden change or disappearance is a reason to notify your medical team immediately.
In the first weeks, it is generally recommended to avoid:
- Measuring blood pressure on the arm with the fistula;
- Blood draws or IV line placements on the same arm;
- Tight clothing, bracelets or watches over the fistula area;
- Sleeping positions that put weight on the operated arm.
Simple exercises (such as repeatedly squeezing and releasing a rubber ball) can speed up vein maturation, but the timing and intensity should be agreed with your doctor.
When Is the Fistula Ready for Dialysis
The fistula is not used immediately after surgery. It needs time for the vein to widen and its walls to strengthen. Maturation usually takes between 4 and 8 weeks, sometimes longer.
Before the first dialysis puncture, the doctor examines the fistula and may use Doppler ultrasound to confirm that blood flow is adequate. The goal is for the first dialysis sessions through the fistula to proceed as safely as possible, with minimal risk of complications.
Possible Complications: What You Should Know, Without Panicking
Every surgical procedure carries some degree of risk, and the arteriovenous fistula is no exception. It is useful to know the most common complications so that you can recognise them early:
- Stenosis: a section of the vein narrows and blood flow through the fistula decreases. You may notice that the thrill feels weaker or that dialysis sessions become harder to complete.
- Thrombosis: a clot forms inside the fistula and blocks circulation. The thrill disappears suddenly and the fistula can no longer be used as an access point.
- Failure to mature: the vein does not dilate sufficiently despite the passage of time, making puncture difficult or unsafe.
- Venous aneurysms: excessive dilation of segments of the vein, usually at repeatedly punctured sites.
Early identification of these problems allows interventions that can save the fistula and avoid the need for a new vascular access.
What are the options if problems arise with the Fistula?
Depending on the type of complication, the doctor may recommend different solutions:
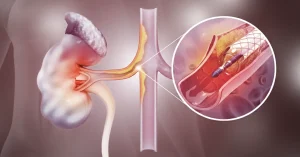
- Balloon angioplasty (fistuloplasty): a catheter with a small balloon is introduced through a fistula puncture to the narrowed area, which is then dilated.
- Surgical revision: a new procedure to repair or reconstruct a section of the fistula.
- Creation of a new access: in situations where the original fistula can no longer be salvaged or no longer provides adequate flow.
The choice of method depends on the results of investigations (for example, ultrasound, angiography) as well as the patient’s general condition.
Warning Signs: When to Contact Your Doctor Immediately
It is important to seek medical help quickly if you notice:
- The thrill can no longer be felt or changes suddenly;
- The arm with the fistula becomes red, hot or very swollen;
- Intense pain develops in the fistula area;
- A puncture site bleeds more than usual and the bleeding does not stop easily;
- Repeated difficulties arise when using the fistula for dialysis.
These symptoms may indicate stenosis, thrombosis or infection. Early intervention can make the difference between a salvaged fistula and the need for a new vascular access.
Frequently Asked Questions About Living with an Arteriovenous Fistula
A well-maintained fistula can function for years, sometimes over a decade, but it requires monitoring and adherence to daily care recommendations.
In general, walking, light exercise and moderate movement are encouraged. Direct blows to the fistula area and contact sports or activities that compress the arm should be avoided.
Yes, provided you have access to a dialysis centre and follow the recommendations related to protecting your arm. It is important to carry your relevant medical documents and information about your dialysis appointments.
Do not wait for it to pass on its own. Contact your dialysis team or doctor as soon as possible to be assessed and to find out whether the fistula can be saved.